While they aren’t dangerous, milia – tiny, hard white bumps no bigger than a pinhead – are still quite annoying to deal with. These small spots can crop up across your body (especially on eyelids and cheeks, and even your abdomen or genitalia), and can be a challenge to banish for good. If you’re closely examining your skin and curious to know if you’re contending with milia, read on. We’ve got all the answers to your milia questions below, including what causes them, how long milia last, the best milia removal treatments, and how to treat milia.
What are Milia?
Milia are small, white, superficial cysts that are filled with keratin – a thick and resilient protein that’s found in skin tissues, hair, and nail cells. It’s easy to confuse milia with whiteheads because of their appearance, but whiteheads are soft comedones filled with a mixture of bacteria, debris, and sebum. Milia are harder, sit on the surface of the skin, and often (though not always) occur in multiples.
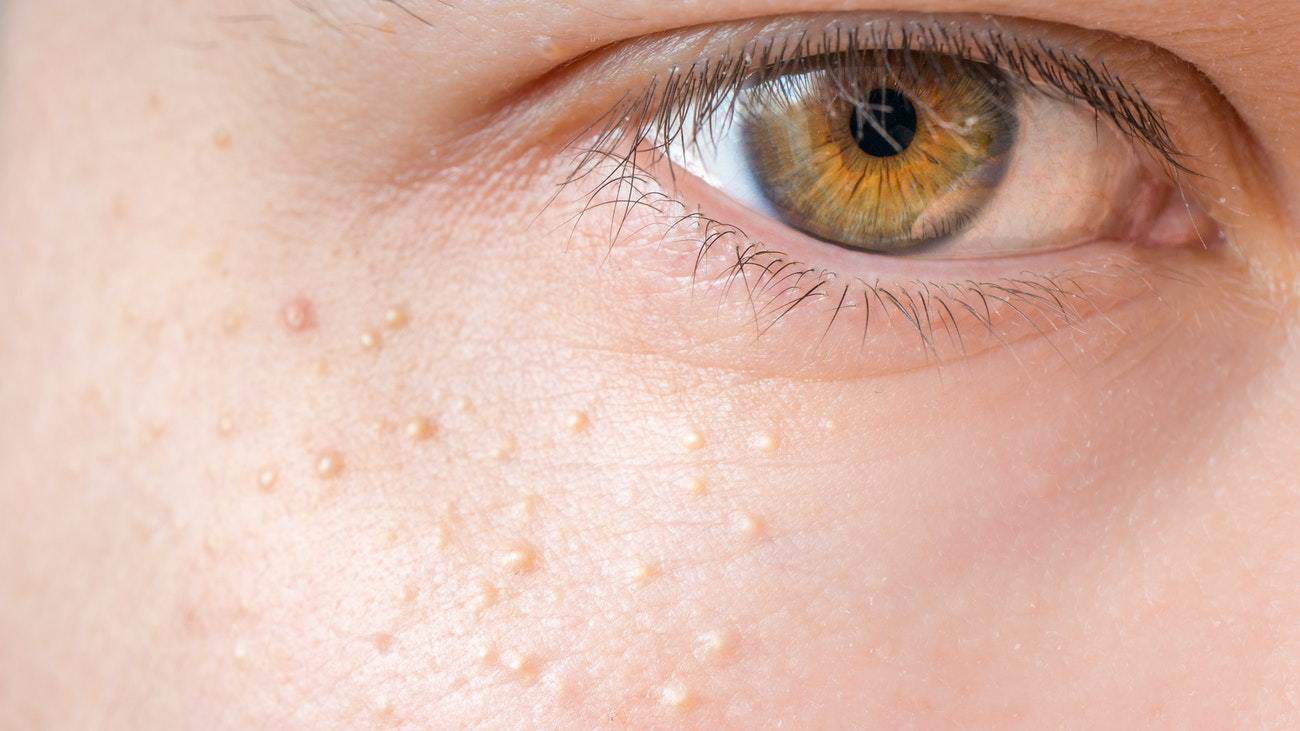
“Milia are completely harmless, usually don’t cause any irritation or pain, and often they will go away on their own after some time,” says Sandra Lee, MD, a board-certified dermatologist who you might know better as Dr. Pimple Popper®. She does, however, concede that milia are frustrating for those who have them. “They may feel like they are unsightly, and also it can be disconcerting when you run your fingers over your skin and feel these firm, very small bumps,” she adds.
While people of all ages and ethnicities can develop milia, some are more prone to dealing with this skin issue than others because of their genetics. If you’re dealing with milia, you’ll likely see this skin concern cropping up throughout your family tree. Other genetic causes of milia include disorders like lupus, Gardner syndrome, and nevoid basal cell nevus syndrome. As mentioned, these tiny cysts can occur anywhere on the body, but milia on the face – including milia on eyelids – is especially common.
How to Get Rid of Milia
If you’ve dealt with milia for a while, you might feel like dealing with the skin issue is a lost cause. Don’t give up just yet, though. Milia removal is possible – just so long as you don’t pick! “Though it might seem tempting, these little cysts are under a layer of skin that is thicker than that of a whitehead,” Dr. Pimple Popper warns. “You can really risk infection and scarring if you try to remove them yourself.”
When left untreated, milia will often go away within a few months, but exfoliating ingredients can help expedite this process. For example, a topical retinoid, such as Obagi Medical 360 Retinol, or an AHA or BHA, such as Herbivore® Prism 12% AHA + 3% BHA Exfoliating Glow Serum, will speed up the skin turnover process. Physical exfoliators, like SkinCeuticals® Micro-Exfoliating Scrub, can help too.
EDITOR’S NOTE: Retinol shouldn’t be used by women who are pregnant, considering getting pregnant or nursing. Please consult with your doctor before use.
If milia really bother you (or you’re feeling too impatient to wait a few months for them to clear up on their own), then it’s best to connect with a board-certified dermatologist for milia removal. Your dermatologist will properly clean the area and excise the little pearl-like bits trapped under the skin in a safe, sterile environment using thoroughly sanitized tools. Typically, milia are removed by using a sterile needle to create a tiny incision, allowing for very careful extraction. Again, do not do this at home; leave it to the professionals! You risk potential infection and scarring when DIYing milia extraction – an arguably worse fate than milia themselves.
How to Prevent Milia from Developing
The approach to prevention is almost identical to milia removal: exfoliation is key. “I recommend using a chemical exfoliant two to three times a week on your face, neck, and chest,” says Deanne Mraz Robinson, MD, board-certified dermatologist and co-founder of Modern Dermatology® in Connecticut. She’s a fan of using the Skinbetter Science® AlphaRet® Peel Pads, as well as a retinoid or the plant-based alternative, bakuchiol. “These treatments keep dead skin cells on the move and pores open, so keratin will not become trapped and milia formed,” she explains.
Dr. Robinson also notes that sun damage has been linked to milia formation – just another reason to dutifully apply your favorite SPF. Remember, even if you mostly spend time indoors, windows still leave you exposed to the sun. Be sure to slather yourself with your go-to sunscreen every day in the name of protecting your skin, from both harmful UVA/UVB rays and milia. If you have more questions about your specific case of milia, we highly recommend reaching out to your provider – they can best analyze your unique needs and work with you on a customized treatment plan.